When Surviving Cancer is Not the End of the Fight: Mollie’s Story
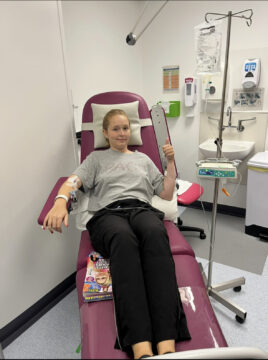
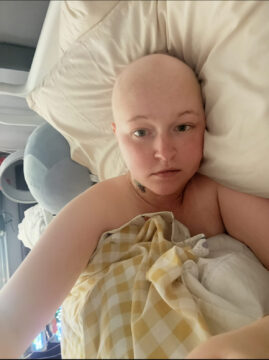
At 24 years old, Mollie was diagnosed with stage 4 diffuse large B cell lymphoma.
Over the months that followed, she underwent more than 800 hours of intensive chemotherapy and spent over 150 days in hospital. The treatment saved her life. Because of the urgency and severity of her illness, there was no opportunity to preserve her fertility before treatment began. She was told that this could be revisited once she was well enough.
Today, Mollie is in remission and has been given an excellent prognosis. She is expected to live a full and normal life. After everything she endured, she is rebuilding that life and beginning to feel like herself again.
However, her fertility has been severely impacted as a direct result of chemotherapy.
The Hidden Consequence of Life Saving Treatment
Following treatment, Mollie’s ovarian markers initially appeared to recover. Her consultants explained that this pattern is well recognised in young adult cancer survivors. The ovaries can temporarily overcompensate after chemotherapy before entering a rapid and often irreversible decline.
That decline is now taking place.
Mollie is currently part of a clinical trial investigating fertility outcomes in young adult cancer patients. Her pre chemotherapy blood results provide a clear baseline of ovarian function before treatment. Using this evidence, her medical team can objectively demonstrate the extent of fertility loss caused directly by chemotherapy.
She is now pursuing a third appeal with her local Integrated Care Board. However, appeals take time. She has been warned that she may not have that time.
There remains a narrow window in which egg freezing or embryo creation may still be possible. Further delay risks removing that option entirely.
The Emotional Impact of Reproductive Loss
The impact of cancer treatment has extended far beyond Mollie’s physical recovery.
Mollie has always wanted to be a mother. Surviving cancer made that hope even more significant. It became a symbol of life, continuity and the future she fought so hard to remain part of.
She has regained her health. Yet she now faces the possibility of losing the chance to build a family.
Alongside this, the long term effects of chemotherapy have significantly altered her professional life. Due to immune system damage following treatment, she was forced to leave her career as a teacher. She is now trying to establish a small business that fits around her ongoing health limitations. However, she is not eligible for a loan or traditional financial support.
She is doing everything she possibly can to move forward, yet continues to face barriers beyond her control. At times, it feels as though everything is stacked against her despite her absolute best efforts.
The emotional toll of this cumulative impact has been profound. This is not about convenience or preference. It is about confronting multiple, life altering consequences of treatment that was necessary to save her life.
A Wider Systemic Issue
Mollie’s case is not isolated. She is involved in a public campaign highlighting systemic gaps in fertility care for young cancer survivors.
Her story has been featured by the BBC, including an interview with Victoria Derbyshire. She has spoken in Parliament with Ashley Dalton and senior representatives connected to the Secretary of State for Health.
There has been acknowledgement that her situation is unjust. However, she has been told that existing policy cannot be changed for an individual case.
The result is that a predictable consequence of cancer treatment is not being met with a timely and equitable response.
Why FNUK Is Sharing This Story
At FNUK, we believe that survivorship must include quality of life. That includes access to appropriate fertility care where treatment has directly caused harm.
Mollie’s experience highlights the urgent need for:
- Clear and equitable national fertility preservation pathways for cancer patients
• Time sensitive appeals processes
• Emergency or exceptional funding mechanisms
• Greater consistency across Integrated Care Boards
• Psychological support for reproductive loss following cancer
Surviving cancer should not mean facing another irreversible loss because of administrative delay or funding barriers.